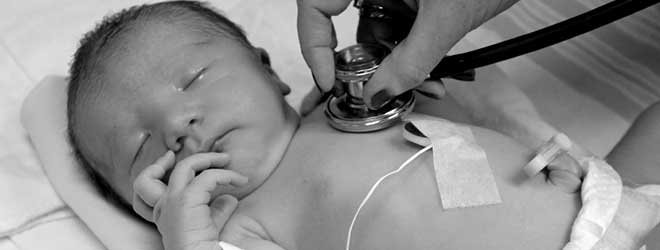
Respiratory failure is the leading cause of death among newborns. In most cases, the basis for this is persistent pulmonary hypertension in the newborn (i). Persistent pulmonary hypertension of the newborn, commonly referred to as PPHN, is a complication in newborn infants that can be life-threatening. PPHN is sometimes referred to as persistent fetal circulation, or PFC. PPHN is a complication in an infant’s heart and lung function. This condition can severely compromise a newborn’s health and can result in long-term complications if left uncontrolled. Severe PPHN occurs in approximately 2 out of every 1,000 live born term infants (ii).
Where You On Prescription Medications While Pregnant?
Call Today for a Free Case Evaluation!
What causes Persistent Pulmonary Hypertension in the Newborn (PPHN)?
PPHN usually occurs within 12 hours after the infant is born. When infants are in utero, they do not use their lungs to breathe. Instead, they receive oxygen from the placenta. PPHN occurs when the infant’s body does not adjust to breathing air after birth. This causes the infant’s blood to bypass the lungs, which sends the blood back to the heart in an oxygen-poor state. As a result, other organs in the newborn’s body are deprived of oxygen and can be seriously damaged.
 Some causes of PPHN include stress while in utero from maternal diabetes, high blood pressure, or other issues. It can also result from congenital conditions, illnesses after birth, or from the infant being deprived of oxygen during the birth process. In recent years, PPHN has been linked to pregnant women’s use of prescription medications that were originally thought to be safe for use during pregnancy. These medications include: Celexa, Depakote, Effexor, Lexapro, Paxil, Pristiq, Prozac, Wellbutrin and Zoloft.
Some causes of PPHN include stress while in utero from maternal diabetes, high blood pressure, or other issues. It can also result from congenital conditions, illnesses after birth, or from the infant being deprived of oxygen during the birth process. In recent years, PPHN has been linked to pregnant women’s use of prescription medications that were originally thought to be safe for use during pregnancy. These medications include: Celexa, Depakote, Effexor, Lexapro, Paxil, Pristiq, Prozac, Wellbutrin and Zoloft.
The “Usage in Pregnancy” labels on many of these medications had to be updated to include an additional warning discussing the possibility that infants exposed to these medications in late pregnancy may have an increased risk for persistent pulmonary hypertension of the newborn (PPHN) (iii).
What are the signs of PPHN?
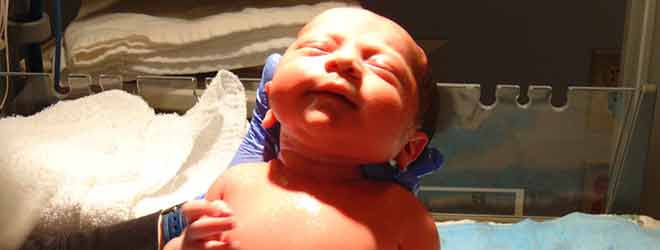
PPHN usually develops within 12 hours of birth, but can last for varying amounts of time depending on the severity of the PPHN. Symptoms of PPHN include: rapid breathing or heartbeat, respiratory distress (evident by signs of flaring nostrils and grunting), and a bluish tinge to the child’s skin. For newborns having trouble breathing or exhibiting signs of poor oxygen delivery, a number of imaging and lab tests will be performed to determine possible causes. Chest x-rays, ultrasounds of the heart, and blood tests can be used to diagnose PPHN.
Additionally, infants with PPHN are born with Apgar scores of 5 or less at 1 and 5 minutes. Most babies with a PPHN diagnosis require treatment in a neonatal intensive care unit. Early treatment for these newborns is important as the primary therapy is supplemental oxygen, to be delivered through intubation, use of a ventilator, or major surgery (iv). As the newborn improves with treatment, he or she will then be slowly weaned off of the oxygen and ventilator support. Outlook for this course of treatment is good considering that approximately 80% of newborns with PPHN can be treated with, and successfully weaned from mechanical ventilation (i).
What are the complications from PPHN?
 PPHN is a gravely serious condition because the newborn’s organs are deprived of oxygen and can be severely damaged as a result. This can cause heart failure, kidney failure, seizures, and even death. Even with treatment and appropriate therapy, the mortality rate for infants with PPHN is estimated to be anywhere from 5-10% (v). Typically, the condition will last anywhere from a few days to several weeks with successful treatment. Some of the long-term effects can be seizure disorders, neurological problems, developmental delays, and hearing loss.
PPHN is a gravely serious condition because the newborn’s organs are deprived of oxygen and can be severely damaged as a result. This can cause heart failure, kidney failure, seizures, and even death. Even with treatment and appropriate therapy, the mortality rate for infants with PPHN is estimated to be anywhere from 5-10% (v). Typically, the condition will last anywhere from a few days to several weeks with successful treatment. Some of the long-term effects can be seizure disorders, neurological problems, developmental delays, and hearing loss.
Sources:
- (i) CHEST Journal. 1988.
http://www.journal.publications.chestnet.org/data/Journals/CHEST/21575/638.pdf - (ii) New England Journal of Medicine. 2006.
http://www.ncbi.nlm.nih.gov/pubmed/16467545 - (iii) Massachusetts General Hospital. 2012.
http://www.womensmentalhealth.org/ssris-and-pphn-the-fda-revises-its-warning/ - (iv) The Regents of the University of California. 2004.
http://www.ucsfbenioffchildrens.org/pdf/manuals/27_PersPulmHyper.pdf - (v) Pediatric Critical Care Medicine. 2010.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2843001/
